
From Here to Timbuktu
Watch these videos from playwright and director Emilio Williams, a former CNN producer who accompanied Robert Murphy on his 2013 visit to Mali:
* "Crisis: The Kids of Mali," which highlights the work of Mariam Sylla, pediatrics chief at Gabriel Touré Hospital and a leader in the field of caring for children with HIV.
* "A Visit to Kierka House," a look at Murphy's visit to an orphanage for children with physical and mental disabilities in Kampala, Uganda.
* "Northwestern Center for Global Health in Uganda," which features Northwestern adjunct faculty member Concepta "Ceppie" Merry '01 GFSM, an Irish-born doctor who trained under Murphy and founded an HIV/AIDS foundation in Uganda.
Bonnie Miller Rubin is a freelance writer in Flossmoor, Ill. As a Chicago Tribune reporter for 25 years, she specialized in health and family issues.
Tell us what you think. E-mail comments or questions to the editors at letters@northwestern.edu.
Find Us on Social Media
Physician Robert Murphy facilitates research and training programs in the developing world as director of Northwestern’s Center for Global Health.
Even for a global citizen like Robert Murphy — with more than 100 trips to Africa under his belt — going to Timbuktu was a gamble.
In 2013 the Feinberg School of Medicine professor traveled to this remote city in northern Mali to assess damage to the country’s already precarious medical facilities following an 18-month reign of terror imposed by jihadists linked to al-Qaida. Reaching his destination from the capital city of Bamako required driving 100 miles along no road — just tire tracks gouged out in the sand. Then he waited on the banks of the Niger River for a boat that might — or might not — arrive, leaving him vulnerable.
No one could quite figure out how the infectious disease specialist managed to enter the “red zone” — unofficially off-limits to all but French military and United Nations personnel. The U.S. State Department certainly was not amused, later responding with a stern reprimand and banning him from the country for a year.
“I never felt like I was in danger. … Obviously, the U.S. Embassy didn’t agree with me,” he says. “But how often does a medical scientist get to witness directly what happens in a war zone?”
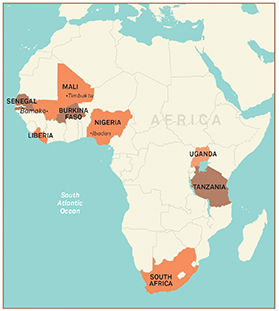 Such risks exemplify Murphy’s commitment to the larger issue of improved health care in sub-Saharan Africa. As director of Northwestern’s Center for Global Health, he oversees research and training for 22 projects in nine countries in Africa and the Middle East, many with some of the lowest survival rates in the world. (In Africa, Northwestern’s Center for Global Health runs programs in Burkina Faso, Liberia, Mali, Nigeria, Senegal, South Africa, Tanzania and Uganda. See map at left.)
Such risks exemplify Murphy’s commitment to the larger issue of improved health care in sub-Saharan Africa. As director of Northwestern’s Center for Global Health, he oversees research and training for 22 projects in nine countries in Africa and the Middle East, many with some of the lowest survival rates in the world. (In Africa, Northwestern’s Center for Global Health runs programs in Burkina Faso, Liberia, Mali, Nigeria, Senegal, South Africa, Tanzania and Uganda. See map at left.)
It is the center’s mission to address the complex issue of health inequities through research and interdisciplinary education initiatives around the developing world. Murphy ’81 GME, ’84 GME, the John P. Phair Professor of Infectious Diseases at Feinberg and professor of biomedical engineering at the McCormick School of Engineering, oversees every aspect of the CGH operations, from competing for federal grants to helping students fill out their visa applications.
Most of all, the center works closely with Feinberg students, residents and faculty to engage in cutting-edge initiatives, such as training the next generation of HIV researchers in Mali, preparing Nigerian universities to expand their own biomedical engineering departments or developing better diagnostic tests to slow and stop hepatitis C continentwide.
It’s difficult for Americans to comprehend the grinding poverty and devastation in places like Mali, where the life expectancy is just 58 years (21 years less than for the average American) and 11.5 percent of kids don’t reach their fifth birthday — a mortality rate almost 17 times higher than in the United States. (Watch the Center for Global Health video "Crisis: The Kids of Mali.")

In the aftermath of the al-Qaida–led invasion of Mali, almost 500,000 people were forced to flee from their homes, causing a massive humanitarian crisis. Photo by Emilio Williams.
For Murphy, such glaring disparities are commonplace. But that detour into Timbuktu revealed a snapshot that even he found unsettling: electricity working just a few hours a day; water delivered by bucket every morning for showering and flushing. The lone hospital had been ransacked by jihadists, and everything with a plug was either stolen or destroyed. The single ambulance, which had been commandeered to transport weapons, had been demolished. In the entire country of nearly 17 million, medical personnel were scarce, with only one doctor to serve every 9,100 citizens, a situation that remains the same today. (The U.S. ratio is one to 400.)
Turning a blind eye to marginalized populations, however, is an option we can no longer afford, explains Murphy. “We are living in a very small world that is growing smaller all the time. We are dealing with important health care issues that are universal and can affect anyone, regardless of where they live.”
Getting your arms around an issue as complex as global health may seem daunting, but Murphy only sees possibilities.
“It’s not that difficult to improve human health, especially when focusing on decreasing morbidity and mortality of preventable diseases,” he says. “I have participated and seen the benefits that arise from relatively basic improvements in health care in some of the poorest settings on earth.”
About 125 medical students were involved in center activities last year. Some of those who participated included a first-year Feinberg student who learned about HIV, tuberculosis and malaria treatment at a university hospital in Dakar, Senegal; a medical student who worked in a rural primary care clinic in Guatemala while learning Spanish; and another student who completed rotations in infectious disease and anesthesiology in Cape Town, South Africa, and Berlin, respectively.
“It’s important for them to have such a palpable experience, where health care really matters and improvements and advancements can be observed in real time,” Murphy says.
Typically, Murphy travels about 145 days and logs about 225,000 miles a year. He often works 16-hour days in blistering sub-Saharan heat, living in spartan accommodations, exposed to all kinds of maladies.
Still, despite the harsh environment, there’s really nowhere else this 64-year-old would rather be. He waxes eloquent on the hospitality and resourcefulness of the African people and their ability to be content with so little. He finds moments of lightness in watching children play soccer with a ball made of paper bags or in the gratitude of a mother whose baby has been helped by something as simple as antifungal ointment.

On the side road to Timbuktu, some villages had only one or two families left. Robert Murphy checked on some of these families and provided basic primary care and prescriptions. Photo by Emilio Williams.
Center for Global Health Focuses on Big Picture
When the center launched in 2009, Murphy envisioned an ambitious enterprise that would deploy all of Northwestern’s strengths — teaching, research, collaboration — to the most despairing places on earth.
Seven years after its inception, the center has more requests for its expertise in developing and implementing programs to enhance health care than it can handle. It now receives 90 percent of its funding for research or training projects from the National Institutes of Health, another sign of its viability. Most of all, there’s a “genuine and passionate interest” among students across the University — both undergraduate and graduate — to help people in the developing world live longer and healthier lives.
That often conjures up images of medical missions, with clinicians providing emergency treatment following a disaster. Instead, the Center for Global Health concentrates on the big picture, working with universities overseas to increase access to care and create a research infrastructure, so that the solutions can be country-owned and country-driven.
“In the past, American and other foreign investigators would come, get specimens, take them back to their home-based labs, do the tests and publish some great papers, barely mentioning the people or scientists who provided them,” Murphy says. “Those days are over. Now our goal is to teach the medical establishment in Africa how to do it themselves and how to fund it.”
The center’s office is modest, tucked away on the 10th floor of a Feinberg building on the Chicago campus. No African art or photos of the director with world leaders — just reports, papers and journals stacked everywhere. “I’m a science guy,” Murphy says with a shrug.
It doesn’t take much to get him talking about current projects, such as one started in 2014 in Jos, Nigeria, to develop diagnostic tests for hepatitis C, leading to earlier treatment and prevention. Previously, the test was expensive and could take up to 12 weeks to obtain results — usually from a hospital so distant that one-third of the patients didn’t bother to pick them up. Today, that test is a finger stick with results available in an hour. The cost has plummeted from $100 to $7 — all of which increases the odds of reining in the virus, which claims an estimated 35,000 lives a year in Africa, according to the World Health Organization.
Another example: the development of Nigeria’s first academic biomedical engineering departments, which brings together experts from Feinberg, the McCormick School of Engineering and the Kellogg School of Management to help Nigerian universities train their own biomedical engineers to develop products for HIV/AIDS testing and treatment. Not only will the new tools expand access to care, but biomedical engineering departments will also enable Nigeria to grow its own medical device industry.
“Rob was the first one to see all the connections. … He drew us into his sphere,” says Matthew Glucksberg, director of the Center for Innovation in Global Health Technologies at McCormick, who is leading the Nigerian program along with Murphy and Kara Palamountain ’04 MBA, executive director of the Global Health Initiative at Kellogg. Glucksberg attributes such achievements abroad to Murphy’s ability to “go off and stick with it,” he says. “The people know he’ll be back — probably next month — and if the program collapses, he won’t abandon them.”
From Aviation to Infectious Diseases
Murphy has been intrigued by building things since he was a child growing up in Evanston. He comes from a long line of engineers — his grandfather, a civil engineer, was one of Boston’s early parks commissioners — and Murphy showed an early talent for math and physics.
Murphy attended Southern Illinois University to study aviation but later switched his major and earned a bachelor’s degree in geography in 1974. He went on to earn a bachelor’s degree in biology from Boston University and his medical degree at Loyola University’s Stritch School of Medicine in Maywood, Ill. After medical school he moved to Northwestern for his internship, residency and fellowship in infectious diseases. Almost 40 years later, he’s still here.
Murphy first became smitten with global health as a Peace Corps consultant in the early 1990s. Louis Sullivan, then secretary of U.S. Department of Health and Human Services, dispatched him to West Africa to solve this mystery: Why were so many returning volunteers bringing home HIV?
“It’s no surprise that so many American volunteers — typically single men and women in their 20s — were having sex. … In general, prevention counseling was grossly inadequate,” Murphy says. (The situation later improved, when the U.S. government issued new safe sex guidelines).
“At one time, I admitted more patients to Northwestern Memorial Hospital than any other staff physician. I also signed the most death certificates. It was overwhelming, and the numbers just kept getting bigger and bigger.” — Robert Murphy
Addressing the HIV/AIDS Crisis in Chicago
When Murphy returned to Chicago and joined the Northwestern Medical Faculty Foundation (now the Northwestern Medical Group) as a physician, the situation wasn’t much better. The HIV/AIDS epidemic was rampant, and he cared for gays, bisexuals, intravenous drug users, hemophiliacs and anyone else who walked in the door with this mysterious ailment.
“At one time, I admitted more patients to Northwestern Memorial Hospital than any other staff physician,” including many patients with HIV/AIDS, he explains. “I also signed the most death certificates. It was overwhelming, and the numbers just kept getting bigger and bigger.”
Around this time Murphy started working closely with John P. Phair, the longtime head of Feinberg’s infectious diseases division and an early AIDS research pioneer. “John was there right at the beginning, when hysteria existed at every level. He was calm, rational and treated patients with the respect they deserved. He kept the lid on the pot,” says Murphy, who holds the professorship named for his mentor.
Shift: From Clinician to Researcher in Africa
Being on the front lines, Murphy realized that the need for better care and a cure was so overwhelming that “nobody could handle this just by practicing good medicine.” So he decided to shift his career from clinical work to research, focusing on viral infections, including the development of anti-retroviral drugs and vaccines for HIV/AIDS, tuberculosis and malaria.
In 2004 Murphy was appointed Nigerian country director for the U.S. President’s Emergency Plan for AIDS Relief, a federal program to combat HIV/AIDS, and charged with training thousands of clinical staff in how to prevent, identify and treat the virus. Confronting the epidemic in Africa was no different than in Chicago, he says, “but with 20 times more patients and less than 1 percent of the resources.”
Under his leadership as country director, the PEPFAR program set up 53 clinics across Nigeria, testing and treating an estimated 175,000 patients, which proved to be both extremely challenging and professionally rewarding. “It gave me and my colleagues a chance to participate in the largest public health project in African history.”
Moreover, when he left PEPFAR in 2010, Nigeria’s HIV prevalence had decreased from 5 percent to 3 percent, which translated into hundreds of thousands of saved lives.
Such gains helped burnish Feinberg’s reputation as a leader in understanding and preventing HIV/AIDS, both in Chicago and overseas. In 2008 the journal Science listed Northwestern among the top 10 institutions with the highest impact on HIV/AIDS research, largely due to the efforts of Phair and Murphy. (Read more on Murphy's work on AIDS in Africa."
The Center for Global Health Is Born
At around the same time, a second factor spurred momentum for the creation of the Center for Global Health. J. Larry Jameson, then dean of Feinberg, was becoming concerned about insufficient oversight of students who were doing internships overseas. Jameson wanted to know where they were located, what they were doing — and he wanted it done right. He allocated $2 million for the startup and appointed Murphy its founding director.
Today, global health has grown into its own established and respected discipline — and Northwestern has grown right along with it, ranked in the top tier of institutions by the Universities Allied for Essential Medicines. (No small feat considering that Harvard’s, John Hopkins’ and Emory University’s global health programs have been around longer and were launched with much larger investments of faculty and staff.) Almost half of all Feinberg students now participate in overseas programs compared with 30 percent nationwide, according to the American Association of Medical Colleges — a metric in which Murphy takes enormous pride.
Three years ago, as an undergraduate in biomedical engineering, Matt Doerfler ’13 worked on a project in Nigeria that illustrates the kind of kinetic sparks that can fly when talented people join forces.
Doerfler collaborated with Murphy and Taiwo Lawal, a pediatric surgeon at University College Hospital in Ibadan, to find a more cost-effective way to reduce hypothermia in infants following surgery. In the United States, an infant warmer can cost up to $12,000 and uses hundreds of dollars more in disposable products for each procedure, which was simply impractical for hospitals with threadbare resources.
After returning to campus for his senior year, Doerfler continued to work on the project — which turned into a collaboration among Feinberg, McCormick and Kellogg — and resulted in the first NIH grant to span all three schools. Eventually the team created its prototype, which costs less than $50 to build and sells for less than $300. The Joey Kare — as it was dubbed — was able to drive down costs by using an electric board under the patient, rather than heat circulating in a balloon. After a series of revisions, the design was handed to the University of Ibadan, which will soon produce its own models.
As it turned out, the engineering student didn’t just help find a new device but a new calling. “Working with Dr. Murphy taught me how to approach health inequities in a sustainable, ethical and ultimately meaningful manner,” explains Doerfler, now starting his second year at Feinberg.
While innovation like the Joey Kare is the objective, it doesn’t always happen, says Jeanne McDermott, program officer at the Fogarty International Center at the NIH, which has funded many of Murphy’s training programs and studies under its Medical Education Partnership Initiative.
“The best programs do more than provide opportunities for students,” she says. “I want to make sure our efforts build and support capacity in the country and not just make it easier for U.S. researchers. I’m impressed by the way Murphy has brought Nigeria together with Northwestern, so it’s mutually beneficial.”
Jonah Musa ’10 MS echoes McDermott’s sentiments. As a young OB/GYN, he first met Murphy about a decade ago in Jos, Nigeria, and followed him back to Northwestern to pursue a master’s degree in clinical investigation. “He creates the kind of environment where all his trainees can succeed,” Musa says. “When you confront him with a problem, his response is: ‘We can and we will fix this.’ He has an open mind and always offers a way forward, which is a rare quality.”
Almoustapha Maiga, a virologist in Bamako, has worked with Murphy on several Mali programs and cites his abilities as a problem-solver. The most enduring lesson he’s learned from Murphy? “You never fail until you decide to do nothing.”

As soon as the French troops freed the remote city of Timbuktu, Robert Murphy traveled to Mali to assess the damage done to the city’s health infrastructure. Photo by Emilio Williams.
The key to transcending cultures, Murphy says, is taking the time to build meaningful and respectful relationships in the field. There’s no “parachuting in” — one reason he has little use for “medical tourism” and won’t allow any student to participate overseas for less than a month.
“Things usually start slowly,” he says. “Then, somewhere around the third or fourth time you come to a new site, people begin to trust you. By that time, you should know what the people really want and need — which may not necessarily be what you thought they wanted or needed.”
As an example of good intentions gone awry, he offers one of his own initiatives to reduce anemia by prescribing iron supplements. While the anemia rate decreased, the malaria rate soared, thanks to all those new red blood cells, which only made humans more attractive to mosquitoes.
But for all his listening and diplomatic skills, Murphy is not afraid to step on some toes, when necessary. Sometimes, that means replacing an in-country scientist with someone more competent. Other times, it might be a tussle with the U.S. Embassy, such as the one that followed his tour of Timbuktu, where he had been invited on previous occasions — before scheduling conflicts, then jihadists derailed his plans.
Such obstacles, of course, are the norm — especially in Africa. Over the years Murphy has endured everything from dysentery to dehydration to nasty bouts of malaria. “Definitely no fun,” he says, “and the prophylactic treatments can make you sicker than the diseases you are trying to prevent.” That was followed by a serious eye infection, called trachoma, which resulted in a two-year regimen of ocular steroids.
Illnesses aside, there are other occupational hazards, which he tends to downplay. Consider the time 10 years ago in Nigeria, when bandits appeared out of nowhere brandishing guns and demanding money. (He fled the vehicle, hiding in the bush until it was safe). More recently in Mali, his hotel was shot up by terrorists, but only after he checked out. “Timing was on my side.”
Still, he expects to wind down within the next five years, retiring from what he sees as a young person’s game.
Looking back over a four-decade career, Murphy is proudest of his role in the PEPFAR program, training more than 100 academic investigators who have become key scientists in their respective countries, and, of course, founding the Center for Global Health.
Given the increasingly global nature of our lives, he believes that the treatment of diseases and medical interventions must also be global.
“In the West we have a false sense that the AIDS crisis is over,” says Murphy. “It’s not over in Africa, and until we have a cure, it’s not over at home either.
“Beyond AIDS, in a global world, infectious diseases know no boundaries, no country of origin, no class, no race: SARS, Ebola, Zika, whatever will come next. This is why creating the health care infrastructure is Africa is as important as sustaining our own infrastructure at home. We’re all in on this together.”



 Facebook
Facebook Twitter
Twitter Email
Email


