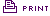
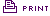 |
The magnitude 7.0 earthquake that hit Haiti on Jan. 12 killed 230,000 people, injured 300,000 and left more than 1 million homeless. Nearly four months after the earthquake hit, John Flaherty, an infectious disease physician and professor at Northwestern’s Feinberg School of Medicine, traveled to Port-au-Prince, the capital and hardest hit area of Haiti, to join other U.S. and Canadian volunteer doctors and nurses working under the direction of the International Medical Corps at the city’s Hôpital de l’Université d’Etat d’Haiti, or University Hospital. Flaherty, who volunteered through Feinberg’s Center for Global Health, worked in the Haitian hospital’s intensive care unit for two weeks. Here are excerpts from his journal, which his daughter, Medill School of Journalism sophomore Maura Flaherty, compiled for Northwestern magazine.
 Day 1: Arrived in Port-au-Prince. The airport is a mass of humanity jostling for space. The trip to the Plaza Hotel is mind-boggling — crazy traffic; colorful trucks and buses loaded down with people; rubble and debris on the side of the road. The hotel is an armed encampment. We’re housed in the conference room. Found an empty cot and set up my mosquito net. Domino’s pizza for dinner in honor of a bunch of people leaving in the morning.
Day 1: Arrived in Port-au-Prince. The airport is a mass of humanity jostling for space. The trip to the Plaza Hotel is mind-boggling — crazy traffic; colorful trucks and buses loaded down with people; rubble and debris on the side of the road. The hotel is an armed encampment. We’re housed in the conference room. Found an empty cot and set up my mosquito net. Domino’s pizza for dinner in honor of a bunch of people leaving in the morning.
Day 2: Up early for a bowl of cereal and lukewarm milk. Off to work at 6:45 a.m. on the IMC bus. A wild ride to the hospital — amazing we don’t hit anybody. Armed guards open the gates to University Hospital — the primary public hospital for the entire country. I meet my team in the ICU. They’re breaking me in slowly — just a couple of patients to follow and lots of help. I’m working with a hospitalist from California, a nurse-practitioner and two nurses from Washington, D.C. — very good people. Boy, is it hot.
Day 3: The hospital is a disaster. It’s like Cook County Hospital on steroids — various doctor and nurse groups on strike, limited or no supplies, erratic garbage collection, nonfunctional toilets, no running water and a completely dysfunctional clinical laboratory system.
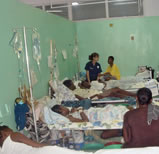 The people are very grateful for whatever we do, which is not very much. I am now the only physician covering the day shift in the 18-bed ICU. Very, very sick patients. I doubt we will be able to discharge half of them alive.
The people are very grateful for whatever we do, which is not very much. I am now the only physician covering the day shift in the 18-bed ICU. Very, very sick patients. I doubt we will be able to discharge half of them alive.
Most of the doctors drip with sweat all day. A couple of fans help a bit, but we try to keep them on the patients. The power goes out all the time. Yesterday the power went out for four to five hours, and the generator — which powers the ventilators and a couple of emergency lights — was out for much of that time. I use a flashlight off and on all day.
Day 4: Lots of discussion at dinner tonight about exactly what we’re accomplishing here. Some folks are really unhappy. It’s hard to see the benefit of what we can do — “spitting in the wind” kind of thing. I try to focus on making a positive impact on whomever I’m with. I hope I can just communicate that I care, even if there’s not much I can do.
Too many gruesome stories: gunshot wound to the arm, bricks to the head, industrial grinders chewing up hands, a couple of deaths today (all patients in their mid-20s) and lots of very advanced HIV/AIDS. … OK, enough of that.
Day 6: Our advanced HIV patients continue to deteriorate with little hope, but no deaths in our ICU today. So, all in all, a pretty good day.
The lack of basic supplies is still hard to accept: no running water, no linens — I mean no sheets, no towels, not even any rags — no cleaning supplies, just yuck. But I got a shower today (yeah!), and the mattress on the floor is an improvement over the cot (I tuck in the mosquito netting to keep the mice out).
Day 7: A 20-year-old woman who was buried in the rubble of the quake for four days, rescued and hospitalized for three months, living for the past few weeks with members of her church because the rest of her family was killed in the quake, has developed acute onset left-sided headache and right-sided weakness. She has no fever, no stiff neck, and she’s awake and talkative. It might be an intracerebral hemorrhage or a brain abscess or a tumor, but no way to know without a CT scan of the brain. But those cost $250, and her fellow church members don’t have that. If she doesn’t improve quickly, we will pass the hat among the doctors and nurses and see if we can raise the money.
Our return to the hotel tonight was delayed with the first of many arrivals from a tap-tap accident. Tap-taps are the Haitian version of public transportation. It’s not uncommon to see an ancient truck painted in bright colors and tricked out in flashing lights and crammed to the gills with people. There are no seat belts, and the back of the vehicle is open so riders can jump onboard. Ejections are not uncommon. In the accident today, 15 people were ejected, resulting in a (literal) busload of blunt trauma.
Day 8: Lots of drama with the Haitian doctors trying to reoperate on a critically ill boy with typhoid. Extensive foot dragging: surgery residents disappearing for hours. And strict adherence to protocol: two units of blood administered in preparation for surgery, but the anesthesiologist wanted only one unit infused and one on hold for surgery! The Haitian doctors at University Hospital refused to take him to the OR. Our night-shift doctors arranged to transfer him to Project Medishare for Haiti’s field hospital for emergency surgery, but the ambulance driver locked his keys in the ambulance. (“Sorry, we can’t go.”) The night-shift staff was on the phone with our IMC leaders requesting permission to break the window of the ambulance (permission denied). Some clever person ultimately jimmied the ambulance door, and off the driver went with our young patient.
Day 9: Difficult start to the day — awakened about 4 a.m. with some gastroenteritis. Not sure how I got it (only drank bottled water, and the only fresh vegetables I ate were the mostly peeled cucumbers). Our attempts to get a head CT scan on the 20-year-old survivor of days buried under the rubble of the quake were unsuccessful. The CT facility failed to answer repeated phone calls. The patient blew one pupil last night, the other pupil this morning and died at 10 a.m. Since we have no neurosurgeon available at the moment, the CT scan probably would not have affected her outcome, but it was frustrating and very sad nonetheless.
We have three patients in the ICU being treated for tetanus. Tetanus is a clinical diagnosis (that is, there is no laboratory test to confirm the diagnosis), so it’s difficult to be certain. Together with the 11-day-old baby with opisthotonus (whole body spasms characteristic of tetanus) that I saw in the pediatric tent, I have seen four possible cases of tetanus in a few days. In the 27 years since I graduated from medical school, I had previously seen exactly one case of tetanus. (Anyone considering not vaccinating their children would reconsider after seeing one of these folks.) The Haitian pediatric residents hoped to transfer the infant to our unit, but I didn’t think it was in the baby’s best interest to be cared for by me, who knows nothing about caring for newborns. So we transferred the baby to the pediatric ICU at Médecins Sans Frontières Spain.
On a happy note, the boy with typhoid was successfully transferred to Project Medishare, where they promptly operated on him. He’s reportedly doing great today. A couple of patients in the ICU who we were convinced would die in a few days have (miraculously?) turned around. Not sure if it was anything we did, but the day and night shift ICU teams were congratulating each other at sign-out tonight.
We have a consensus among the medical staff that Haitians are probably the toughest people we have ever seen. They rarely request pain medication, never seem to be concerned about personal privacy (an impossibility in this setting anyway) and accept bad news (often terrible news) as a fact of life. Several family members have pointed to heaven and told me, “It is in God’s hands.”
Spirituality is an important element of life here. We have visitors throughout the day who circulate among the patients, praying and singing. They don’t seem to know any of the patients but undertake a spiritual ministry to the sick.
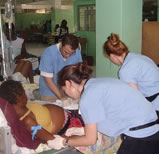
Day 10: Feeling much better today. The 11-day-old baby with tetanus transferred to MSF France is reportedly doing well. (Yes!)
Our ICU is not a very pleasant place and not so fragrant (especially when the power is out and the fans aren’t working). The upside is that we have two or three nurses who move constantly among the patients and two dedicated Haitian translators who not only help us communicate but hold patients during procedures and console patients and families. The nurses never stop working.
Day 11: Early on I was called over to assess a possible case of tetanus in an older man. I was told his limbs were contracted and stiff and that he was unresponsive. As I arrived to evaluate him, he died very suddenly, and his limbs relaxed. His family did not seem particularly surprised, but they were unhappy with the prospect of paying the morgue for the release of his body. A few minutes later I looked up to see three of his family members awkwardly hustling his body out the back door. So many tragic and funny moments here — sometimes simultaneously.
Day 12: About midnight a young man walked his brother into the ER. He was a 20-year-old male with a dry cough, fever and “stiffness” and who had had difficulty walking without assistance for several days. He had a high fever and was minimally responsive. I was convinced he had severe malaria, but two rapid malaria diagnostic tests were negative. The young man looked really bad, so we started treatment for malaria, meningitis and tetanus. He became more unresponsive and developed progressive respiratory distress. Several portable ventilators were available, but the consensus here is not to intubate anyone likely to require mechanical ventilation for longer than 24 to 48 hours. The place is not equipped to sustain support for too long, and we have never been successful with prolonged ventilation in the past. Chris, Meg and I decided the asthmatic woman we had just intubated in the next bed was more salvageable. So the young man was given comfort care and died 90 minutes later — bleeding from his nose and mouth and IV sites — a sad, weird, puzzling case. I only hope he wasn’t the first case of some horrendous epidemic. His brother remained at his side throughout. When we explained through our translator that we could not save his brother, he sobbed and chanted at his side until he expired. His death really affected Meg, an emergency medicine doctor from New York. It was her last shift and such a sad way to finish her work here.
Day 14: My last shift — I’m relieved but feeling a bit guilty. As bad as things are here, the immediate impact of the earthquake has abated at the hospital, and by all reports the situation here in some respects is better than before the earthquake. However, more than a million remain homeless. Almost none of the children or adults we have cared for have received basic childhood vaccinations. The HIV rates here are comparable to the hardest hit areas of sub-Saharan Africa. It’s a public health nightmare.
I’m ready to go home. An exhausting, exhilarating, frustrating, inspiring experience. I hope I can take some of the lessons I have learned here and bring them home with me.
Follow-up: The International Medical Corps and its doctor and nurse volunteers withdrew from the hospital over subsequent weeks at the request of the University Hospital administration, transitioning care back to Haitian health care providers. The intensive care unit was closed because the Haitians did not believe they could continue to provide that level of care. Medical care returned to a strict fee-for-service model, restoring some revenue for Haitian doctors and hospitals but significantly limiting access to care for most Haitians.
Comments. Questions. E-mail the editors at letters@northwestern.edu.